VT in Structural Heart Disease
What is VT?
Ventricular tachycardia (VT) refers to an abnormal rapid heart rhythm originating from the heart’s lower chambers. This often arises as a result of abnormalities of the heart muscle that accompany heart attack, heart failure, and other heart diseases that alter the structure of the heart.
How does VT occur in structural heart disease?
In structural heart disease, VT results from an abnormal electrical circuit involving a region of scar in the heart’s lower chambers.
Prior heart attack is the commonest reason, and refers to a previous blockage in the blood supply to the heart muscle and the resulting damage to that heart muscle deprived of oxygen and nutrients. Other heart conditions such as heart failure can also result in scarring within the lower chambers of the heart.
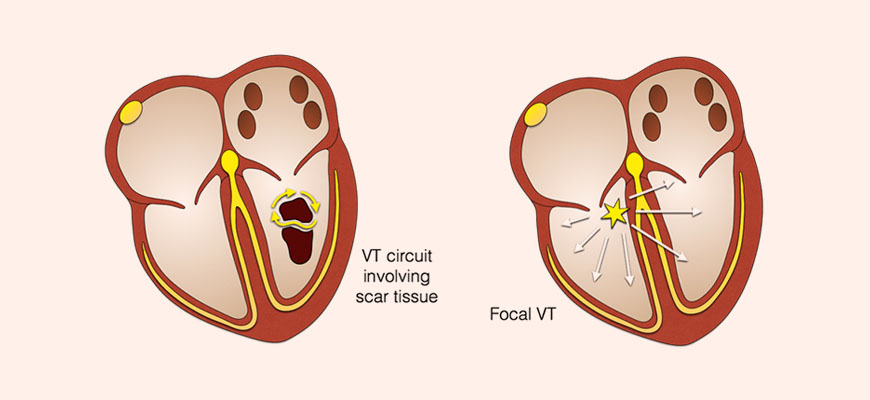
Strands of healthy tissue within these scarred regions provide the opportunity for abnormal electrical short circuits to occur. A short circuit is normally triggered an ectopic beat that gets caught up within the scar.
The resulting VT circuit overrides the normal heart rate, usually at over 130 beats per minute and sometimes at over 200 beats per minute. This is called “re-entry VT”, because the electrical circuit re-enters the scar with each heartbeat only to exit again to generate the next heartbeat.
Less often, VT results from a small cluster of cells that has developed the ability to fire spontaneously. This abnormal focus of excitable cells may send out a series of rapid electrical impulses, resulting in “focal VT”.
What are the consequences of VT?
During an episode, you will usually be aware of the rapid beating of your heart. Other symptoms might include dizziness, breathlessness, sweating, chest pain, and anxiety.
The most severe symptom of VT is blackout. It is a dangerous situation usually reflecting complete failure of the heart to pump. This is called cardiac arrest, and is different to “heart attack” which refers to a blockage in the heart’s arteries, although a severe heart attack can cause cardiac arrest.
Cardiac arrest results from any combination of the following:
- The VT is so rapid that the heart chambers have insufficient time to fill and eject
- The VT causes severe incoordination of the heart muscle wall during ejection
- The heart muscle is very weak due to pre-existing heart disease
- The VT electrical circuit degenerates to complete electrical chaos or ventricular fibrillation (VF)
In many cases, cardiac arrest is unlikely to correct itself and requires medical resuscitation involving CPR and an electric shock to the chest to reset the heart’s electrical system. Individuals who have an ongoing risk of developing dangerous VT may benefit from an implanted cardiac device called a defibrillator or ICD that can detect a cardiac arrest and deliver a life-saving shock.
What tests do I need if I have VT?
You may require the following initial tests.
- Blood tests – To determine if there is an underlying condition that has provoked your arrhythmia, such as thyroid or electrolyte disturbances and to check the condition of your liver and kidneys.
- ECG – To evaluate your heart rhythm.
- Holter monitor – To evaluate your heart rhythm over a 24 h period. If you are in normal rhythm, this may reveal ventricular ectopic beats, episodes of VT, or other arrhythmias that correspond with your symptoms. This may also reveal episodes of arrhythmia which you are unaware of.
- Echocardiogram – To evaluate the structure and function of your heart.
- Cardiac MRI – To examine the heart in fine detail. To identify regions of scarring the heart’s lower chambers – these are not usually visible on echo
- Coronary angiogram – To evaluate the blood supply of the heart.
Learn more about the different Heart Tests here.
How is VT treated in structural heart disease?
There are several options:
- Treatment of the underlying heart disease only. In all cases, the underlying heart disease must be treated. This will not repair existing areas of scar, but can reduce the future risk of VT. For those individuals having very infrequent and short-lived episodes of VT that are not troublesome, one option is to leave them alone.
- Medications to suppress VT. Medications are sometimes effective at suppressing VT. This will improve symptoms but will not cure the underlying problem. There is the possibility of developing side-effects from these drugs.
- Catheter ablation. If medications are ineffective, catheter ablation may be useful in reducing the future risk of VT. This involves a keyhole instrument called a “catheter” to deliver radiofrequency energy to ablate (destroy) the abnormal tissue responsible for the VT. Success of this approach depends heavily on the severity of the underlying structural heart disease, and the number of potential VT circuits harboured within the scarred tissue.
- ICD implantation. Many patients with structural heart disease are at risk of cardiac arrest and would benefit from implantation of an internal cardiac defibrillator. This is the most effective method of restoring normal heart rhythm after the development of life-threatening VT or VF and is akin to having an ambulance crew accompany you 24 h a day.